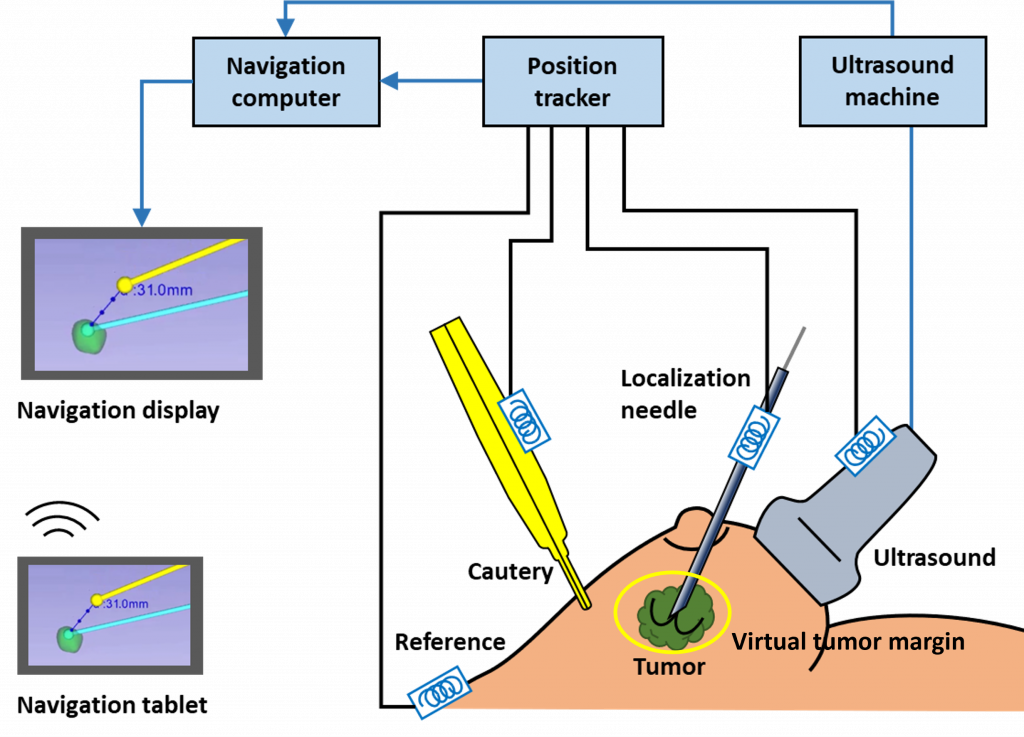
Our research focuses on using advanced imaging and navigation systems to improve the accuracy of medical procedures across fields like cardiology, breast cancer, radiation therapy, and virtual reality, leading to better patient outcomes.
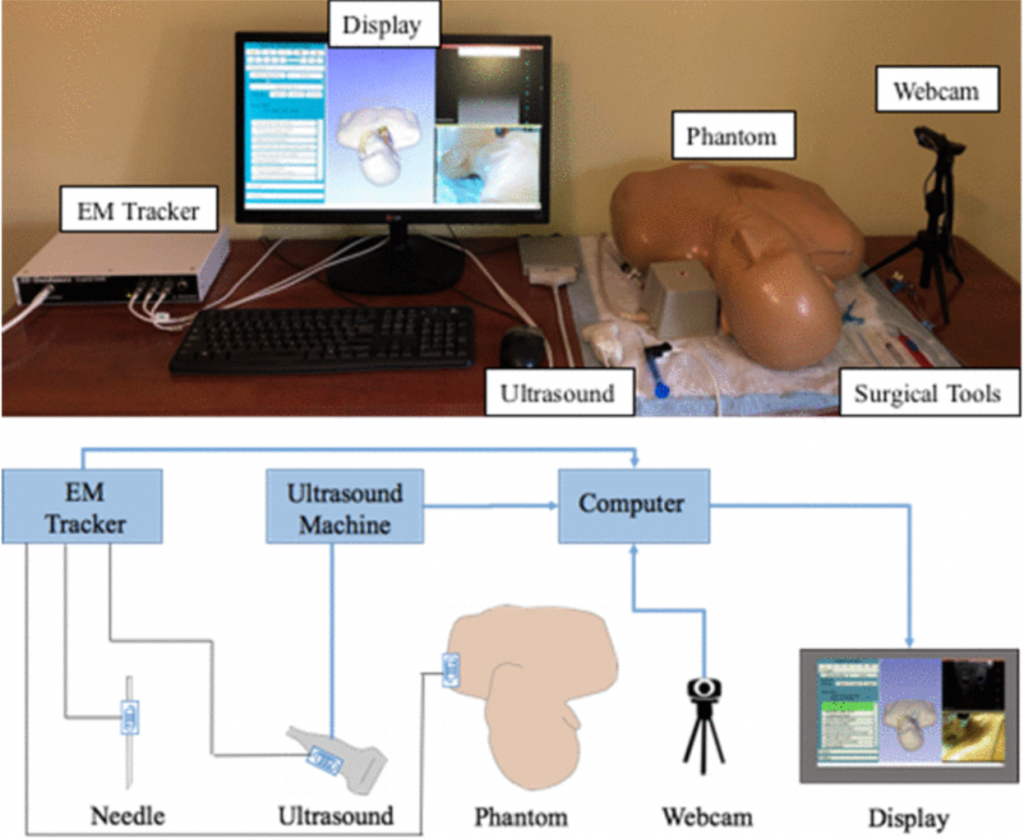
Medical education has shifted to competency-based learning, where training focuses on skill proficiency rather than traditional apprenticeship. Our lab collaborates with the Faculty of Health Sciences to develop simulation-based curricula, improving student experience and earning international recognition for our contributions to medical education advancement.
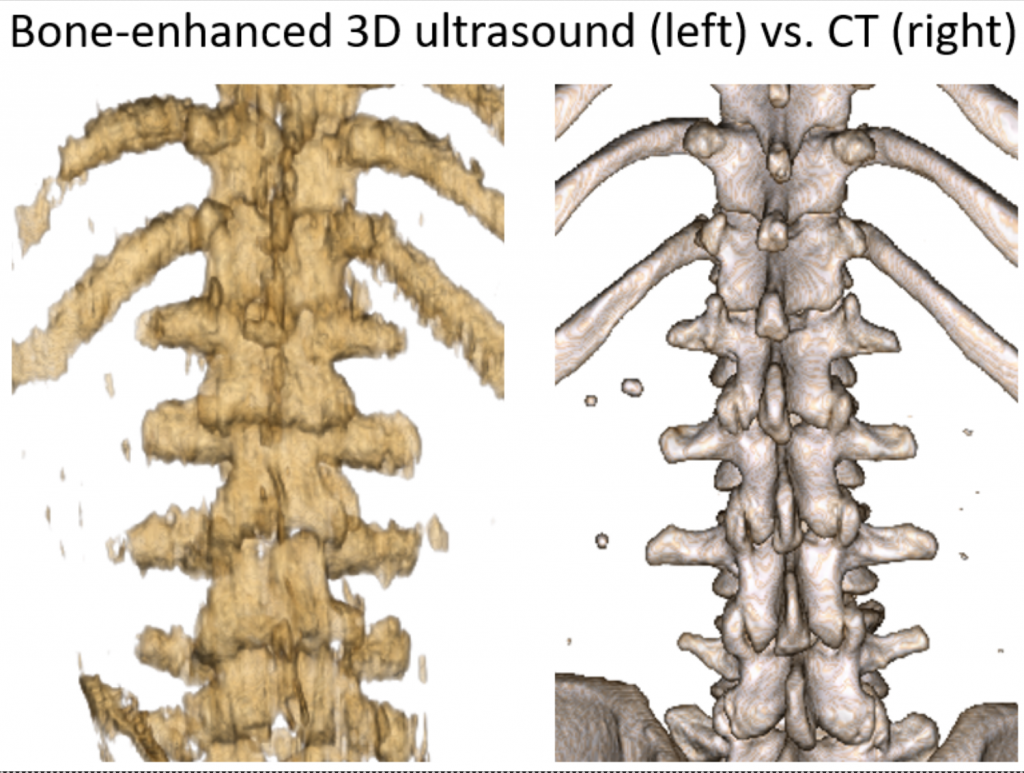
Artificial intelligence has transformed medical imaging, quickly and accurately analyzing large amounts of data to detect subtle abnormalities in ultrasound, MRI, and CT scans, aiding in early disease detection. Our group develops AI solutions and incorporates them into systems for guiding procedures and training, demonstrating their significant impact on healthcare diagnostics and treatment planning.